Newborn screening success
The government backed Newborn Bloodspot Screening (NBS) program has successfully found two cases of Congenital Adrenal Hyperplasia (CAH) in Victorian babies since starting screening in July this year.
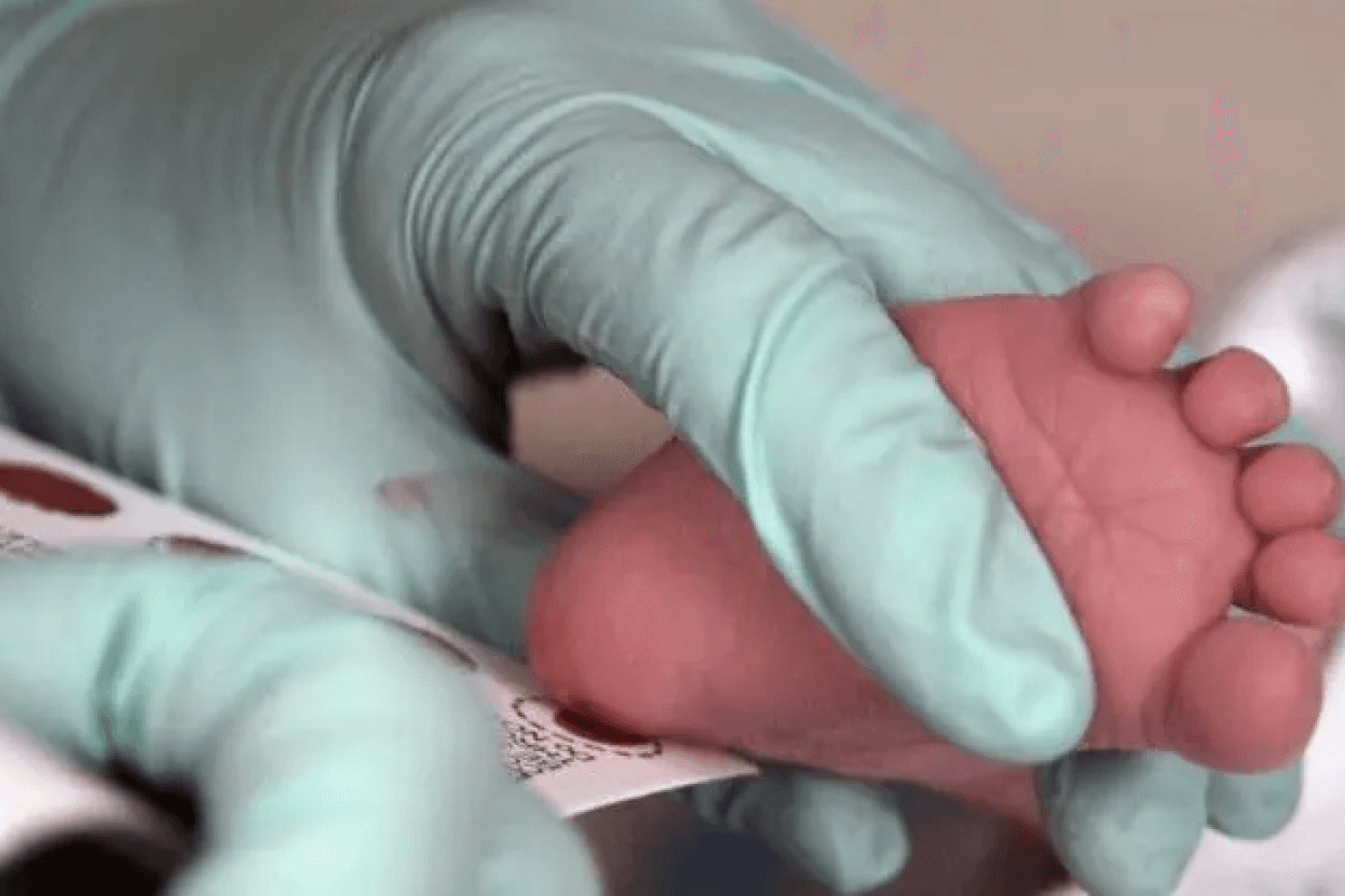
A newborn pilot program screening for genetic conditions that limit hormone production in the adrenal glands has already uncovered two cases since launching two months ago.
The heel prick test, delivered in Victoria by Victorian Clinical Genetics Services (VCGS) in partnership with the Victorian Department of Health, identifies babies that have rare, but serious medical conditions such as cystic fibrosis and hypothyroidism. Early diagnosis allows for timely medical intervention and better treatment outcomes. About one in 1000 babies will be found to have one of these serious conditions. Last year, the Victorian Department of Health announced a $1 million Newborn Bloodspot Screening (NBS) program to develop a pilot project to screen for Congenital Adrenal Hyperplasia (CAH).
The program has successfully found two cases of CAH in Victorian babies since screening started in July this year.
VCGS Deputy Head of Biochemical Genetics Associate Professor Ronda Greaves , who welcomed the funding, said she looked forward to the positive impact this would have on affected babies.
“CAH can be diagnosed through the simple heel prick test and treated through relatively inexpensive medication. If left untreated, newborns can become extremely unwell and may die suddenly in the early weeks of life.”
Health Minister Mary Anne Thomas said the Government was proud to support VCGS in this important work, helping to identify newborns at risk of developing serious illnesses and providing treatment early, "This is another example of how Victoria is providing evidence-based screening and testing to improve health outcomes of newborn babies and their families,” she said.
What is Congenital Adrenal Hyperplasia (CAH)?
CAH affects the adrenal glands, a pair of walnut-sized organs above the kidneys, which produce key hormones that play critical roles in the body’s response to illness and stress. Infants with CAH lack an enzyme required to make these hormones, which can result in very low cortisol and salt levels and dangerously high potassium levels.
What does this mean for Victorian babies?
This funding means Victorian babies with CAH will be identified early and receive care. This reduces the need for emergency care and optimises their treatment options. Currently, CAH is often missed in newborns, as the presentation can be attributed to other more common conditions.
Jack’s story: Before CAH was added to NBS
After Jo and Dan brought their two and a half-week-old baby boy Jack to Bendigo Hospital, he was experiencing a life-threatening health crisis, which caused him to be significantly dehydrated with extremely low levels of salt and high levels of potassium. His heart rhythm was abnormal, and he required intensive care management at The Royal Children’s Hospital. The cause: undiagnosed CAH.
Doctors at the hospital ordered the appropriate tests and diagnosed CAH. Happily, baby Jack recovered well and was discharged home on the necessary medications to replace the hormones and electrolytes needed to treat CAH. He is now five years old and lives a very healthy and active life.
“When diagnoses are delayed, there is not only the significant impact and psychological distress to the family of their newborn baby becoming very unwell, but there is also a high economic and healthcare resource burden of such an admission. This can be prevented through NBS,” said Dr Michele O’Connell, consultant endocrinologist at The Royal Children’s Hospital.
VCGS is committed to providing and continually improving screening and diagnostic testing for Victorian babies and families. Working in partnership with the Victorian Department of Health to include serious genetic conditions like CAH on the NBS program embodies this mission and supports quality care.